A new study from the Workers Compensation Research Institute delves into the reasons why back surgery rates vary widely for workers in different states, with Oklahomans nearly three-times as likely as Californians to go under the knife.
The finding that back surgery rates vary across states is not entirely new. WCRI studies consistently report that the odds of injured workers having back surgery depend on the area of the country in which they seek treatment for their back pain.
In the latest study, however, researchers find that certain “local area factors” are correlated with the likelihoods that workers with low back injury have back surgery. “Local are factors” found to increase the likelihood of surgery for workers with back pain include:
- More surgery-intensive local practice norms.In areas where physicians do more surgery are workers who were not injured on the job, they are also more like to operate on workers who were injured at work. (Surgery intensity was measured using surgery rates for workers covered under group health insurance.)
- Higher reimbursement rates for surgery.Here, WCRI measured price differentials between workers comp insurers and group health insurers, which ranged from -$283 (negative, means workers comp pays less) to $10,866 (workers comp paying more). If the workers comp payment was higher by $1,700, the estimated surgery rate climbed 0.7 points higher.
- More surgeons in the area.The average number of orthopedic and neurosurgeons per 100,000 people ranges from 5.3 to 8.3 across states, according to WCRI. If one more surgeon practices in an area, the estimated surgery rate goes up by 0.4 percentage points, the research finds.
The analysis also examines case-mix factors, such as wage levels, gender, injury type and severity, finding, for example, that men, construction workers and those with higher incomes are 2-4 percent more likely to have surgery, and that surgery is 10 percent more likely for workers with severe back injuries.
But what is telling is that the “local area factors” contributed to the variation in back surgery rates, even after controlling for case mix. This is not true for knee surgery, a less controversial surgery, which WCRI researchers studied for comparison purposes. “Local area factors” explained little of the variation in knee surgery rates, while case-mix factors were highly important in explaining knee surgery propensity, the WCRI report says.
Explaining the importance of the findings, WCRI notes that roughly one-fifth of the injuries covered by workers compensation are back injuries.
The findings can be used to shape discussions about second opinions, treatment guidelines, and fee schedules, WCRI suggested in an announcement about the new study.
“This study addresses an important area of inquiry by investigating some of the hypotheses put forward to explain the wide variation in surgery rates. Some of the factors are within the control of workers compensation policymakers. Other factors result from the dynamics and practices of the larger health care system,” said Dr. Christine Yee, WCRI economist and one of the authors of the report.
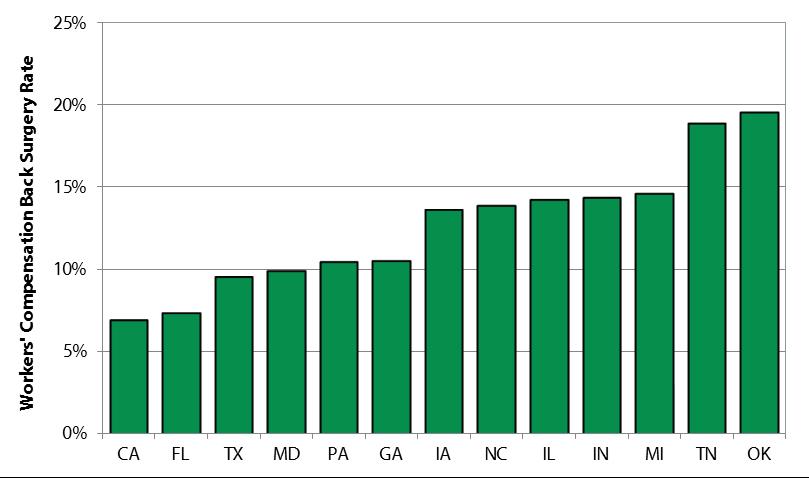
The study analyzed workers in 13 states who had work-related back injuries. Among the states studied, Oklahoma had the highest back surgery at 19.6 percent; California had the lower, 6.9 percent.
With respect to each of the “local area factors,” WCRI reported these findings:
- Corresponding to its low workers comp back surgery rate, California was the state with the lowest local practice norm—the median surgery rate for workers covered under group health insurance. While the median state practice norm is 6.3 percent, California comes in at only 3.8 percent—2.5 percentage points below the median state rate. Iowa is the highest at 10.5 percent, or 4.2 points above the median.
- Michigan has the lowest number of back surgeons, 5.3 per 100,000 people; Iowa is second-lowest at 5.4 per 100,000. In contrast, Maryland has 8.3 orthopedic and neurosurgeons per 100,000 people—1.7 more than the median state figure of 6.6 per 100,000.
- The state with the highest reimbursement margin is Illinois, paying $10,866 more under workers comp than group health. Texas is the lowest, paying more than $5,000 less under workers comp.
Another “local area factor” analyzed in the WCRI is presence of alternative, nonsurgical medicine, which was studied by using the number of chiropractors in an area as a representative measure. WCRI found the surgery rates were lower in areas with greater access to alternatives. Speculating on why, the report said it was unclear why the correlation indicates that patients were cured by alternative practitioners or that the alternative treatments simply bought patients enough time for their injuries to resolve.
Whatever the reason, Iowa tops the charts on alternatives with 41 chiropractors per 100,000 people, compared to a median of 24. Maryland, at the low end, has only 11 chiropractors per 100,000 people.
Source: WCRI




















 USAA Not Done With Dividends: Florida Reforms Prompt $0.5B Payout
USAA Not Done With Dividends: Florida Reforms Prompt $0.5B Payout  The Financial Case for Negotiation: How Indemnity Discipline Can Transform Carrier Economics
The Financial Case for Negotiation: How Indemnity Discipline Can Transform Carrier Economics  Storm Counts, Landfalls and Losses: The Hidden Risk Behind a ‘Quiet’ Hurricane Season
Storm Counts, Landfalls and Losses: The Hidden Risk Behind a ‘Quiet’ Hurricane Season  AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says
AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says 






