States that do not have a fee schedule in place are likely to pay more for workers compensation-related medical services, according to two Workers Compensation Research Institute studies that analyzed the medical price index (prices paid for professional services) and the hospital cost index (payments made for outpatient services).
The two studies examined the impact of fee schedules on prices in workers comp claims. In “WCRI Medical Price Index for Workers Compensation,” Dr. Rebecca Yang analyzed claims with prices paid for professional services during 2002-2012 in 25 states. In “Hospital Outpatient Cost Index for Workers Compensation,” Dr. Yang reviewed hospital outpatient payments related to surgeries made during 2005-2010 in 20 large states.
“We’re looking at actual prices paid by workers compensation payors,” said Dr. Yang.
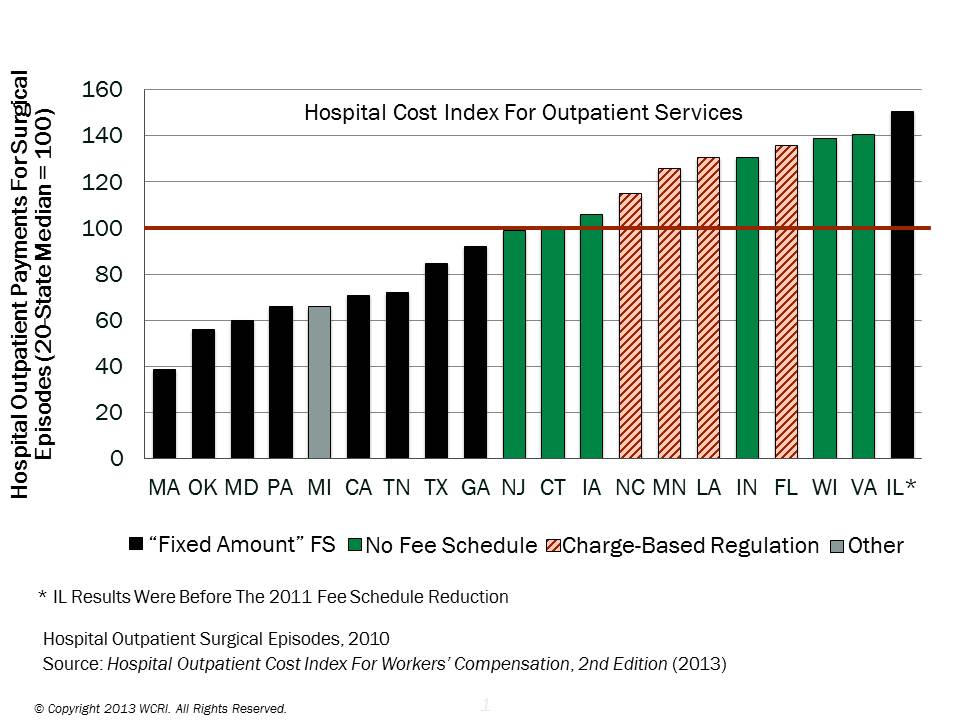
The WCRI researcher found that fee schedules do affect pricing and that fees paid for professional services varied greatly. States that did not have fee schedules had higher professional services and hospital outpatient payments, while states that had a fixed-amount fee schedule paid less.
According to the study, the median states were Louisiana and Arizona. Wisconsin recorded the highest prices paid for professional services, as “prices paid were 100 percent higher than among the 25 studied states,” Dr. Yang said, while Florida reported the lowest prices paid for professional services, at “30 percent lower than in the median state.”
The WCRI outlined four types of hospital outpatient fees:
- Fixed—majority of states
- Charge—four states
- Other—one state
- No fee schedule—six states
 According to the studies, prices paid for nonhospital services increased more rapidly in states without fee schedules.
According to the studies, prices paid for nonhospital services increased more rapidly in states without fee schedules.
States with charge-based fee schedules for hospital outpatient services had higher payments. Dr. Yang cited Florida as an example, indicating the charge-based fee schedule did not constrain payments.
In Texas, where multiple fee schedule reforms were enacted between 2003 and 2008, the prices paid during that time mirrored the reforms.
“Prices paid tracked fee schedule reforms made,” Dr. Yang said.
(This article was originally published in Claims Journal. Reporter Denise Johnson is the editor of Claims Journal)




















 With Customer Reviews Increasingly Polarized, Communication Is Key: Trustpilot
With Customer Reviews Increasingly Polarized, Communication Is Key: Trustpilot  The Race for California Insurance Commissioner: Meet Jane Kim
The Race for California Insurance Commissioner: Meet Jane Kim  10 Year Study Finds No Real Benefit to Common Knee Surgery
10 Year Study Finds No Real Benefit to Common Knee Surgery  Executive Viewpoint: One AI Won’t Save You
Executive Viewpoint: One AI Won’t Save You 




