Workers compensation insurers aren’t getting the large aggregate volumes of COVID-related claims projected during the early months of the pandemic, but different data sources give varying readouts on developments for individual U.S. states and classes of workers.
In fact, while claim frequencies are down for workers compensation overall with business shutdowns bringing lower numbers of non-COVID claims, and while the bulk of COVID comp claims are short-duration low-dollar claims, some insurers have paid out claims that were $2 million or more for health care workers infected on the job. And the length of tail of COVID-related comp claims is far from certain, experts said during a webinar last Thursday.
In a single week in January, Teresa Bartlett, chief medical officer for Sedgwick, said more than 10 people called her who had tested positive for COVID last summer. “They were young people in their 30s. Suddenly sitting at their desks working, [they] developed shortness of breath, really severe headaches and profound [levels] of hypertension, just out of the blue,” she reported during the opening minutes of the webinar, “COVID Claims Development: Workers Compensation and Beyond.”
Bartlett was responding to a question about the long-term effects of COVID posed by Kimberly George, global head of Product Development and Innovation for Sedgwick, who co-hosted the webinar with Mark Walls, vice president of Communications and Strategic Analysis with Safety National. (The event was the second 2021 installment of the Out Front Ideas webinar series regularly presented on workers comp issues by the Safety National and Sedgwick.)
Reporting on the results of a study of 4,000 people in the U.S., Bartlett said that 50 percent were unable to work full time six months after they tested positive for COVID, even though only 8 percent of those people actually were hospitalized.
She reported on symptoms ranging from fatigue to attention disorders to breathing difficulties based on a larger volume of research, noting that 80 percent of 50,000 patients infected with COVID develop one or more long-term symptoms. (See related sidebar, “What Long-Term COVID Looks Like”)
While the symptoms, for the most part, might keep people out of work rather than contributing to a workers comp claim, she said, “We don’t know quite yet from the literature if this virus is lying dormant in the tissue for a little while and then suddenly something activates it. There’s more that we don’t know than what we do know,” expressing particular concern to health care workers. These front-line workers who resiliently keep going on the front lines every day may be suffering from PTSD. “I’m a little worried what will happen with these folks. It’s something we have to be very mindful of in our industry and be prepared for how we will deal with it,” she said.
Walls noted that workers comp claims data for health care workers is one of the categories that’s largely missing from data reported by the National Council on Compensation Insurance, which hosted its own webinar in January 2021. (Related articles: Responding to the Impact of COVID-19 on Workers Compensation and It Could Have Been Worse. An Update on COVID-19 Impact on Workers’ Compensation)
A significant portion of the health care industry is self-insured, he said, explaining that self-insureds, for the most part, do not report their data to any of the bureaus. Displaying a chart from the Bureau of Labor statistics that shows the top 20 industries by employment nationwide, he highlighted the education sector as well as federal, state and local governments as other sectors of the economy that are mostly self-insured, collectively representing over 30 percent of the jobs in the top 20 industries.
Walls also noted that while NCCI covers most states, it does not cover the largest states, including California and New York. NCCI’s data represents less than half of all workers compensation data nationwide, he said.
During the webinar, Alex Swedlow, president of the California Workers Compensation Institute, filled in the one of the gaps, reporting recent data for California. Max Koonce, chief claims officer for Sedgwick, and Tim Stanger, a vice president in the claims department of Safety National, were able to provide data on the self-insured businesses. Safety National is largest provider of excess coverage for qualified self-insured entities, Stanger said.
California’s Experience
Swedlow started off, noting the scary early multibillion-dollar California comp estimates coming out in the second quarter of last year.
Reporting on actual COVID-19 infections and deaths in the state and actual workers comp claims, he said that injured workers between the ages 18 and 65 made up about 78 percent of our state’s infections and about one-quarter of all the fatalities. The actual number of workers compensation claims was a small fraction. Only about 4.7 percent of the working-age Californians who were infected had a corresponding workers compensation claim, and roughly 5.6 percent of the fatalities among working-age Californians had an accompanying workers compensation claim, he said. “This shows you just how wrong those original estimates were by focusing on what we all thought was a reasonable proxy, the working-age Californian.”
Swedlow also drilled down into comp claims data by industry, noting a change in the distribution of claims for the first half of 2020 claims compared to more recent claims—from October 2020 through January 2021. In the earlier time period, 39 percent of these COVID-related claims were from the health care sector compared 29 percent more recently. While the percentage of claims from first responders (“public safety/government workers”) stayed around 15-16 percent in both time periods, retail workers now represent 12.5 percent of infections compared to 7.9 percent in first-half 2020, and transportation workers are 8 percent of the total, double what they were earlier in the year.
Self-Insured Classes and WFH Claims
Stanger and Koonce both reported waves of claims in April, July and December of last year, with a December frequency peak surpassing earlier levels.
Overall, Safety National’s claims, excluding the COVID claims, were down 26 percent from 2019, Stanger said, after revealing that public entities, health care networks and educational institutions account for 50 percent of the insurer’s excess comp book of business. Including COVID claims, the number of claims dropped about 10 percent compared to 2019. Stanger and other panelists said they expect that number to continue to decrease as more claims data gets through reporting systems.
Stanger also presented claims data by age of worker, reporting that 85 percent of Safety National’s claims related to workers aged 20-55 and that the average incurred amount of the claims was roughly $4,300.
In contrast, comp claims for workers over the age of 55 had an average cost more than three times higher—about $15,000—with co-morbidities and other factors complicating the disease progression.
Focusing in on the most severe claims, Stanger said that 63 percent of Safety National’s COVID death claims were for workers over the age of 55, and just over half were in the health care industry. He provided details of four catastrophic health care worker claims, each costing more than $2 million, including one in which the injured person’s reaction to the COVID-19 infection included renal failure, brain injury and eventually quadriplegia.
Counting up all of Safety National’s COVID claims with incurred amounts over $100,000, he said that 15 percent of those were actually above $1 million—”a mix of deaths and extended ICU hospitalizations.”
Koonce said that while only 11 percent of Sedgwick’s total book of business relates to the health care industry, the industry represented half of the firm’s overall claim count.
Breaking down the overall claims by level of severity, he said that 90 percent of Sedgwick’s COVID clomp claims require little medical treatment or time away from work, while another 8 percent are “moderately complex,” involving about six weeks away from work and medical visits costing $3,000 to $5,000.
“The vast, vast majority of claims are of a short duration. Generally, they’re pretty well wrapped up within 60 days,” he said. The severest cases, roughly 1.5 percent, involve significant time away from work—a half a year, on average, involving expensive ICU treatment.
Koonce also said that he sees a higher rate of ICU hospitalizations for workers in the health care industry. “We’re not exactly sure why that is occurring, but it is important to note that it’s a three- or four-point increase over other industries,” he said.
Koonce wrapped up his discussion of COVID comp claims trends, noting that there’s another small pool of workers comp claims emerging from the COVID pandemic. “Although it was a very low number to begin with, we are seeing an increase in the work from home claims,” he said. Those are not “directly COVID claims,” he said, but they are ticking up from a small base, “centering around ergonomic type issues—’my back hurts because I’ve been sitting in my kitchen chair all day,’ those types of things.”





















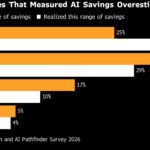 AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says
AI Savings Misses ‘Should Be Making Executives Uncomfortable,’ Bain Says  The Big Dog Is Off the Tech Porch: State Farm as ‘Next Gen Good Neighbor’
The Big Dog Is Off the Tech Porch: State Farm as ‘Next Gen Good Neighbor’  A $10.5 Trillion Cyber Problem: Whose Risk Is It Anyway?
A $10.5 Trillion Cyber Problem: Whose Risk Is It Anyway?  Bending the Casualty Curve: Why Casualty Analytics Is Approaching Its Inflection Point
Bending the Casualty Curve: Why Casualty Analytics Is Approaching Its Inflection Point 








