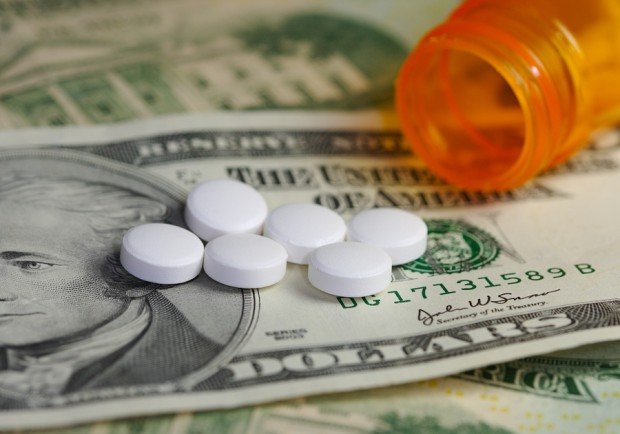
An analysis of pharmacy cost data shows there was an 8.7 percent drop in spending on drugs in 2015 in workers compensation injury cases.
The decline in 2015 is consistent with the overall downward drug cost trend seen over the last six years, which was interrupted by a 6.4 percent rise in 2014, according to the CompPharma annual report.
The CompPharma’s Annual Survey of Prescription Drug Management in Workers Compensation analyzed the 2015 pharmacy cost data of 30 payers including workers compensation insurance carriers, third-party administrators, self-insured employers and state funds.
Larger payers saw greater drops in drug spend and many of the 30 firms surveyed enjoyed double-digit decreases, according to the report.
According to the study, the payers credited tighter clinical management, better integration with their pharmacy benefit managers (PBM)and prescriber interventions for the decrease. All have opioid management programs, according to the study.
“Twenty percent of the respondents also had assertive settlement initiatives and have been closing older claims,” said Joseph Paduda, president of CompPharma. “Overall, payers have seen drug costs go down by 11 percent in the past six years despite the 2014 increase.”
Opioids remained the number-one payer concern with compounds ranking as the main emerging issue.
The participating payers had drug spends ranging from $1.2 million to $200 million and collectively represent about 23 percent of the total workers compensation drug spend. The total workers compensation annual pharmacy spend is approximately $5.5 billion, according to the report.
The author cautions that a payer’s drug cost is not the same as drug price. Price is one component of drug costs to a payer along with the number and type of drugs.
In addition to asking about drug spends, the CompPharma report also asked payers about cost drivers, cost reduction programs, opioids, physician dispensing, emerging issues and PBMs’ performance.
The payers gave mixed reviews to consolidations among pharmacy benefit managers. Some respondents said they hoped mergers would bring better pricing and more clinical capabilities while others expressed concern that the lack of competition would breed complacency.
“There is a sense of acceptance along with a little wariness about potential customer service issues,” Paduda said. “Consolidation in other segments of the industry has spawned customer service problems when people-based operating models were replaced with offshored or tech-enabled models.”
CompPharma is a consortium of workers’ compensation PBMs active in workers compensation.
Source: CompPharma


















 The Race for California Insurance Commissioner: Meet Stacy Korsgaden
The Race for California Insurance Commissioner: Meet Stacy Korsgaden  The Race for California Insurance Commissioner: Meet Steve Bradford
The Race for California Insurance Commissioner: Meet Steve Bradford  The Race for California Insurance Commissioner: Meet Jane Kim
The Race for California Insurance Commissioner: Meet Jane Kim  Automation Theater: Why Carrier AI Investments Aren’t Showing Up in the P&L
Automation Theater: Why Carrier AI Investments Aren’t Showing Up in the P&L